Insulin Bill Would Cap Monthly Supplies of Drug at $50

Audio By Carbonatix
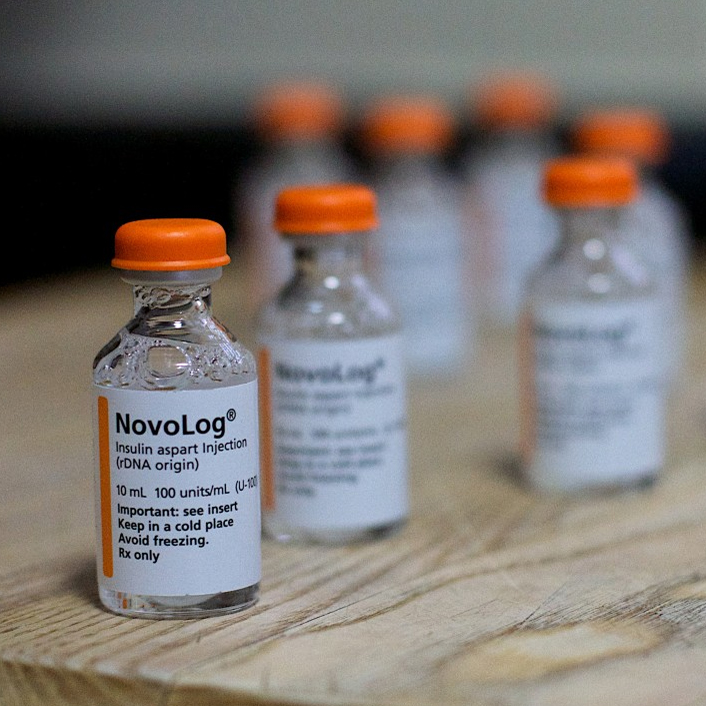
A bill introduced this legislative session would cap the cost of insulin at $50 per month. Courtesy of CTMIrror.org
Proponents say measure has broad support in a short session and is more aggressive than similar efforts in Illinois and Colorado, which capped insulin costs at $100 per month.
By Jenna Carlesso, CTMirror.org
Lawmakers who want to tackle the high cost of prescription drugs in a short legislative session rolled out a bill Thursday that caps the monthly cost of insulin at $50.
The measure is more aggressive than similar efforts in Illinois and Colorado, which last year championed legislation capping insulin costs for users at $100 per month.
Connecticut’s bill also would limit the price of insulin-related supplies, such as syringes, pumps, and blood sugar meters, to $100 a month.
State Rep. Sean Scanlon, a key backer of the measure, said while the actions taken in other states are commendable, Connecticut lawmakers want to go further.
“If we can cap it at $50 a month and be the first state to cap the supplies, I think we would really be helping a considerable number of diabetics afford this lifesaving drug,” he said. “Capping the cost at $100 is great, but $100 is still a lot of money to people.”
As the price of insulin has soared in recent years, people have delayed filling precriptions or switched to alternatives, sometimes with grave consequences.
The Health Care Cost Institute reported that Type 1 diabetes patients – who generally must inject themselves every day – paid an average of $5,705 for insulin in 2016, nearly double what they paid four years earlier.
Under laws passed in Colorado and Illinois, the price of a 30-day supply of insulin is capped at $100. Insurance companies must absorb the balance.
The Colorado law, signed by Gov. Jared Polis in May, also directs the state’s attorney general to investigate how prescription insulin prices are set and make recommendations to the legislature.
Scanlon said he doesn’t believe the cap on insulin would spur insurers to increase premiums. He pointed to companies like Bloomfield-based Cigna, which already has moved to limit the monthly cost of insulin for its members to $25.
“If this is what insurers are saying they can do, then I think we can find a way to do this,” Scanlon said. “I don’t believe they’re going to get up and say this is going to cost them more money and they’re going to raise premiums, because some of them are already doing this voluntarily.”
The legislation also includes a provision giving pharmacists the authority to dispense insulin without a prescription in emergency situations. That portion of the bill is modeled after an effort in Ohio known as Kevin’s Law.
Shortly before New Year’s Day in 2014, Kevin Houdeshell went to pick up an insulin refill, but learned that he needed a new prescription. His doctor’s office was closed for the holiday, and Houdeshell was turned away at the pharmacy.
During the following days, he had high blood sugar that spiraled into diabetic ketoacidosis. Houdeshell’s body was found in his apartment on Jan. 8, 2014 after he didn’t show up for work.
Kevin’s Law, which allows pharmacists to give patients a 30-day supply of a lifesaving drug like insulin even if the prescription has expired, went into effect in 2016. Other states have passed identical legislation.
“It’s all about making sure that this does not happen to anybody in Connecticut,” Scanlon said.
Also included in the bill is a plan to set up an emergency fund for people who can’t otherwise afford the medication. To pay for it, proponents said they would enforce a little known, 20-year-old law requiring nursing homes and Department of Correction facilities to recycle unopened, unexpired prescription drugs. State officials say the recycling program is still operating, but there are no records of fines or enforcement. Facilities that don’t comply may be fined up $30,000 for each violation.
The CT Mirror reported on the recycling program in December. Officials with the Department of Social Services, which oversees the initiative, would not answer questions about whether enforcement checks had ever been conducted.
Lawmakers in both chambers have expressed support for the insulin bill. Senate Democratic leaders featured it in their 2020 health reform agenda, unveiled last month.
“We are committed to the basic idea that nobody in Connecticut should die because they don’t have access to insulin,” Sen. Matthew Lesser, D-Middletown, said.

Logan Merwin, 13, center, tells legislators and the media that he’s long been dependent on insulin and worries about affording the drug when he’s no longer on his parents’ insurance. Courtesy of CTMirror.org
Logan Merwin, 13, told legislators Thursday that he’s had to rely on insulin for Type 1 diabetes most of his life. He worries what will happen when he’s no longer on his parents’ insurance – a reality he may have to contend with sooner if the Affordable Care Act is struck down.
A couple of years ago, his family shelled out more than $700 for one month’s supply of insulin. His mother has put together a medical savings fund so Logan can buy the drug during his young adult years.
“I’ve been worrying about when I’m living on my own with little money, how am I going to get insulin? I’m going to be in this situation in just under 10 years,” said Merwin, a Haddam resident. “I’ve heard my parents on the phone arguing with suppliers because we needed supplies. How am I going to fit that into my working and school schedules?”
Susan Halpin, executive director for the Connecticut Association of Health Plans, which lobbies on behalf of insurers, said insurance company leaders will discuss the issue with legislators. She declined to comment on whether the measure would force insurers to increase premiums, saying she had not yet seen the bill.
“We share the concern about the underlying cost of insulin and many carriers have already undertaken taken measures to help address the issue. That said, we look forward to working with policy makers to see if there’s more that can be done,” Halpin said. “Capping copays, however, doesn’t address the underlying price. It only shifts the burden to the health care premium dollar instead.”
The bill is one of several drug-related proposals the General Assembly will consider this year. Legislators are also exploring the importation of prescription medicine from Canada, the creation of a board to regulate drug prices, and a ban on mid-year changes to drug formularies, among other ideas.
Scanlon said the insulin bill has broad backing. A public hearing on the proposal is scheduled for Feb. 25.
“This is going to be one of the bigger bills we do this session that has near total bipartisan support,” he said. “I think everyone recognizes there’s a legitimate crisis going on when it comes to insulin.”
Reprinted with permission of The Connecticut Mirror. The author can be reached at [email protected].
Like what you see here? Click here to subscribe to We-Ha’s newsletter so you’ll always be in the know about what’s happening in West Hartford!



